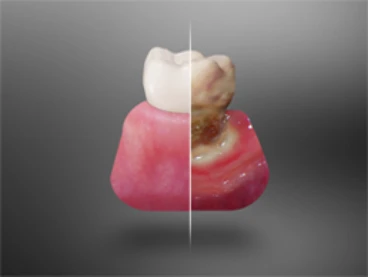
Gum disease is the leading cause of tooth loss in adults — and one of the most common chronic infections in the human body. Yet because it rarely causes significant pain in its early stages, most people don’t realize they have it until it has already caused damage that can’t be undone.
At Magnolia Way Dentistry in Apex, NC, Dr. Wayand and hygienist Laura screen for gum disease at every routine visit, catch it early when it’s most treatable, and provide personalized periodontal care that protects your gums, your teeth, and your long-term health. Whether you’re looking to prevent gum disease or you’re already dealing with its symptoms, this is the right place to start.
What Is Gum Disease?
Gum disease — also called periodontal disease — is a bacterial infection of the tissues that surround and support your teeth. It begins when plaque, the sticky film of bacteria that forms on teeth, is not removed consistently through brushing and flossing. Over time, plaque hardens into tartar (calculus), which can only be removed professionally — and the bacteria within it trigger an inflammatory response in your gum tissue.
Gum disease progresses in stages, and the stage it’s caught in determines how it’s treated:
Stage 1: Gingivitis
Gingivitis is the earliest and most reversible stage of gum disease. It’s characterized by inflammation of the gum tissue — redness, puffiness, and bleeding when you brush or floss. At this stage, no bone or tissue has been permanently lost. Gingivitis is entirely reversible with a professional cleaning and improved home care.
Stage 2: Early to Moderate Periodontitis
When gingivitis is left untreated, the infection spreads below the gumline. Bacteria begin attacking the connective tissue and bone that anchor your teeth in place. Pockets form between the teeth and gums — deeper than the healthy range of 1–3 millimeters — creating spaces where bacteria thrive out of reach of a toothbrush. At this stage, some bone and tissue loss has occurred and cannot be fully reversed, but progression can be halted with appropriate treatment.
Stage 3: Advanced Periodontitis
In advanced periodontitis, significant bone loss has occurred. Teeth may become loose, shift position, or require extraction. Severe gum recession, persistent bad breath, and pain when chewing are common. Treatment at this stage is more intensive and focuses on stopping further destruction and preserving as many teeth as possible.
Why Gum Disease Is More Than a Dental Problem
The connection between periodontal health and overall systemic health is well-established and significant. Chronic gum infection doesn’t stay confined to the mouth — bacteria and inflammatory markers from periodontal disease enter the bloodstream and have been linked to serious health conditions including:
- Heart disease and increased risk of heart attack and stroke
- Type 2 diabetes — gum disease and diabetes have a bidirectional relationship, each making the other harder to control
- Respiratory infections — bacteria from the mouth can be aspirated into the lungs
- Adverse pregnancy outcomes — including preterm birth and low birth weight
- Cognitive decline — emerging research links periodontal disease to increased risk of dementia
Treating and controlling gum disease isn’t just about saving teeth. It’s a meaningful investment in your overall health.
Warning Signs of Gum Disease
Because gum disease is often painless in early stages, it’s easy to miss without professional monitoring. Symptoms to watch for include:
- Gums that bleed when you brush or floss — this is not normal and should never be ignored
- Red, swollen, or tender gum tissue
- Persistent bad breath that doesn’t improve with brushing
- Gums that appear to be pulling away from the teeth (recession)
- Teeth that feel loose or have shifted position
- Pain or discomfort when chewing
- Visible pus between the teeth and gums
- A change in how your teeth fit together when you bite
If you’re experiencing any of these symptoms, don’t wait for your next scheduled cleaning. Contact Magnolia Way Dentistry for a periodontal evaluation — the sooner gum disease is caught, the simpler and more effective the treatment.
How Gum Disease Is Diagnosed at Magnolia Way Dentistry
Gum disease is diagnosed through a combination of clinical examination and X-rays. At every routine visit, Laura — Magnolia Way Dentistry’s hygienist with over 30 years of experience — performs a periodontal assessment that includes:
- Probing — measuring the depth of the pockets between your teeth and gums at multiple points around each tooth
- Recession measurement — noting how much gum tissue has pulled away from the tooth root
- Bleeding on probing — an indicator of active gum inflammation
- Mobility assessment — checking whether any teeth have loosened
- Radiographic bone level evaluation — X-rays reveal bone loss not visible clinically
This data is tracked over time, allowing the team to identify trends, catch early changes before they become significant, and monitor the effectiveness of treatment. Patients always receive a clear explanation of their periodontal health status and what it means.
Gum Disease Treatment Options at Magnolia Way Dentistry
Preventive Care — The First Line of Defense
For patients without gum disease or with early gingivitis, regular professional cleanings every six months are the cornerstone of prevention. Removing plaque and tartar before they cause gum damage — combined with strong home care habits — is the most effective strategy for keeping gum disease from developing in the first place.
Scaling and Root Planing (Deep Cleaning)
Scaling and root planing — commonly called a deep cleaning — is the primary non-surgical treatment for early to moderate periodontitis. It’s a more thorough procedure than a routine cleaning, performed in sections of the mouth (typically one or two quadrants per appointment) under local anesthesia.
Scaling removes plaque and tartar from below the gumline — from the deep pockets that routine cleaning cannot reach. Root planing smooths the root surfaces of the teeth, which removes bacterial toxins embedded in the root and makes it harder for new plaque to adhere. This process allows the gum tissue to heal and reattach to the tooth, reducing pocket depths over time.
Periodontal Maintenance
After completing active gum disease treatment, patients transition to a periodontal maintenance schedule — typically a cleaning every three to four months rather than the standard six. This more frequent schedule is essential to controlling gum disease long-term, because the bacteria that cause it repopulate cleaned pockets within weeks. Periodontal maintenance keeps bacterial levels suppressed, monitors pocket depth and bone levels, and prevents the disease from progressing again.
Antibiotic Therapy
In some cases, Dr. Wayand may recommend topical or systemic antibiotics as an adjunct to scaling and root planing to reduce bacterial populations and enhance treatment outcomes. This is typically reserved for more advanced cases or situations where infection is particularly resistant to mechanical treatment alone.
Gum Disease Prevention — What You Can Do at Home
Professional care and strong home habits work together. The most effective things you can do to prevent gum disease between visits:
- Brush thoroughly for two minutes, twice a day — use a soft-bristled toothbrush and focus on the gumline
- Floss once daily — flossing removes plaque from between teeth and below the gumline where brushing can’t reach
- Consider a water flosser or interdental brushes as a supplement if traditional flossing is difficult
- Don’t smoke or use tobacco — smoking is one of the most significant risk factors for gum disease and dramatically slows healing after treatment
- Manage systemic conditions — particularly diabetes, which significantly increases gum disease risk
- Stay hydrated — dry mouth reduces saliva’s natural cleansing effect and increases bacterial buildup
- Keep your scheduled professional cleanings — skipping appointments allows tartar and bacteria to accumulate
Serving Apex, Cary, Holly Springs & Surrounding Communities
Magnolia Way Dentistry provides comprehensive periodontal care for patients from Apex, Cary, Holly Springs, Fuquay-Varina, and Raleigh. With over 30 years of combined hygiene experience on staff and a thorough, unhurried approach to every exam and cleaning, this is a practice where gum disease is caught early — and managed effectively for the long term.
- Comprehensive periodontal screenings at every visit
- Scaling and root planing for active gum disease
- Customized periodontal maintenance schedules
- Most major dental insurance plans accepted
- CareCredit financing available
Frequently Asked Questions
Yes — bleeding gums are one of the earliest and most reliable warning signs of gum disease. Healthy gums do not bleed during brushing or flossing. Bleeding indicates that gum tissue is inflamed, which is the body’s response to bacterial infection. In its early stage (gingivitis), this is completely reversible with a professional cleaning and improved home care. Persistent bleeding should always be evaluated by a dentist — it is not something to normalize or ignore.
Gingivitis — the earliest stage of gum disease — is fully reversible with professional treatment and consistent home care. Once gum disease progresses to periodontitis, any bone and tissue loss that has already occurred cannot be regenerated through standard treatment, but the progression of the disease can be halted and controlled. This is why early detection at regular checkups is so important — catching gum disease at gingivitis means you can get back to full health. Catching it later means managing a chronic condition.
A deep cleaning — technically called scaling and root planing — is a non-surgical periodontal treatment that removes plaque and tartar from below the gumline, where a routine cleaning cannot reach. It’s recommended when pocket depths indicate that bacteria have established themselves below the gumline and gum attachment has been compromised. If Dr. Wayand or Laura recommends a deep cleaning, it means active gum disease has been detected that routine cleaning alone won’t resolve. It is not an upsell — it is a clinically necessary treatment to stop the infection from progressing.
For mild gingivitis, a single professional cleaning combined with improved home care is often all that’s needed, with resolution typically within a few weeks. For scaling and root planing, treatment is usually completed over two to four appointments — one or two quadrants of the mouth per visit — followed by a re-evaluation four to six weeks later to assess how the tissue has responded. Long-term management through periodontal maintenance continues indefinitely to keep the disease under control.
Scaling and root planing is performed under local anesthesia, so the procedure itself is comfortable — you’ll feel pressure but not pain. Some tenderness and sensitivity in the gums for a few days after each appointment is normal and manageable with over-the-counter pain relievers. The discomfort is temporary and typically far less than patients expect. Routine cleanings for gingivitis are generally no more uncomfortable than a standard hygiene visit.
Research has consistently shown a significant association between periodontal disease and cardiovascular conditions including heart attack and stroke. The leading theories involve two mechanisms: bacteria from the mouth entering the bloodstream and contributing to arterial inflammation, and the systemic inflammatory response triggered by chronic gum infection increasing cardiovascular risk. While treating gum disease has not been definitively proven to prevent heart disease, controlling oral infection is widely considered an important component of overall health management.
Patients who have been diagnosed with and treated for gum disease are typically placed on a periodontal maintenance schedule of every three to four months, rather than the standard six-month interval. This more frequent schedule is essential because the bacteria responsible for gum disease repopulate cleaned pockets within weeks — regular professional removal keeps those levels suppressed and prevents the disease from progressing. Returning to a six-month schedule before the condition is fully stable greatly increases the risk of recurrence.
Yes. Brushing alone does not remove all plaque — particularly from between the teeth and below the gumline. Without consistent daily flossing and regular professional cleanings to remove hardened tartar, gum disease can develop even in people with good brushing habits. Other factors like genetics, tobacco use, diabetes, certain medications, and hormonal changes also increase susceptibility regardless of home care quality. This is why professional monitoring at every dental visit matters even for patients who feel their home care is thorough.









